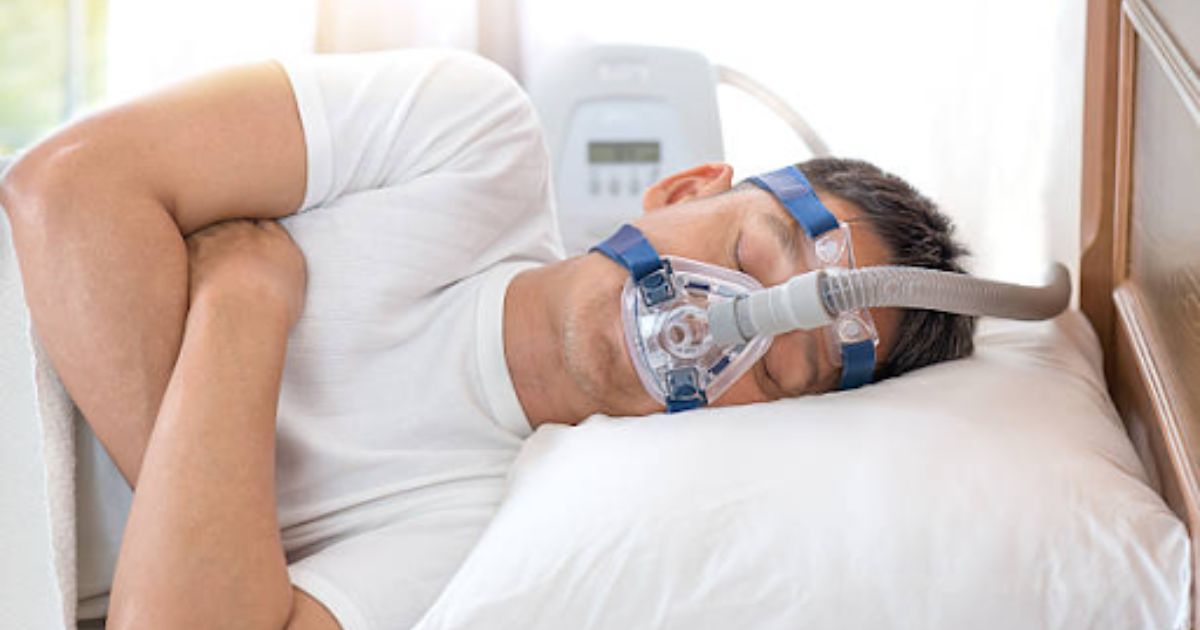
Sleep apnea is a common sleep disorder characterized by brief interruptions in breathing during sleep. These interruptions, known as apneas, can lead to a range of health issues, including daytime fatigue, cardiovascular problems, and even cognitive impairments. Managing sleep apnea is essential for overall well-being, and understanding factors that can worsen the condition is crucial. In this comprehensive guide, we will explore 8 factors that can make sleep apnea worse and offer insights into how to mitigate their impact.
1. Obesity
One of the most significant risk factors for sleep apnea is obesity. Excess weight, especially around the neck, can lead to the narrowing of the airway, making it easier for the airway to collapse during sleep. This in turn increases the frequency and severity of apneas. Additionally, adipose tissue, commonly found in individuals with obesity, releases inflammatory substances that can further aggravate the upper airway’s condition. To combat these adverse effects, losing weight through a combination of diet and exercise can be an effective way to reduce the severity of sleep apnea in overweight individuals. This may include consultation with a registered dietitian to create a tailored diet plan, engaging in regular physical activity to shed excess pounds, and tracking progress under the guidance of a healthcare provider.
2. Alcohol and Sedatives
The effects of alcohol on sleep apnea are noteworthy. When alcohol is consumed, it acts as a depressant on the central nervous system. This means it relaxes the muscles, including the muscles that keep the airway open. As a result, individuals with sleep apnea may experience more frequent apneas and louder snoring after alcohol consumption. Similarly, sedative medications, including tranquilizers and some sleeping pills, can have a muscle-relaxing effect on the airway. This muscle relaxation can lead to an increased likelihood of apneas during sleep. Therefore, for individuals who enjoy an occasional drink or require sedative medications for other health issues, such as mental health, it’s essential to discuss these habits with a healthcare provider. They can provide guidance on the timing and dosage of medications or recommend lifestyle modifications to minimize the impact on sleep apnea.
3. Smoking
The link between smoking and sleep apnea is well-established. Smoking tobacco introduces a multitude of harmful chemicals into the body, including nicotine and tar. These substances can have detrimental effects on the respiratory system, leading to inflammation and damage to the upper airway tissues. If you’re a smoker and have sleep apnea or are at risk of developing it, quitting smoking should be a top priority. Smoking cessation programs, nicotine replacement therapy, and support from healthcare providers can all be valuable resources in your journey toward better health and improved sleep.
4. Sleeping Position
The relationship between sleeping position and sleep apnea is rooted in anatomy. When you lie on your back, gravity pulls the tongue and soft palate toward the back of the throat. This can partially or entirely block the airway, resulting in apneas or snoring. In contrast, sleeping on your side can help keep the airway more open and reduce the likelihood of obstruction.
Positional therapy is a non-invasive approach to managing sleep apnea that focuses on encouraging side sleeping. Several devices are available, ranging from simple body pillows to more advanced positional therapy aids that alert you when you shift onto your back during sleep. Before using any positional therapy device, it’s advisable to consult with a sleep specialist or healthcare provider to determine its suitability for your specific needs. Additionally, combining positional therapy with other sleep apnea treatments, such as continuous positive airway pressure (CPAP) therapy, may provide optimal results for some individuals.
5. Nasal Congestion
Nasal congestion and sleep apnea share a complex relationship. When your nasal passages are congested, it can create a situation where you’re more likely to breathe through your mouth during sleep. Mouth breathing can lead to an increase in airway resistance and airflow turbulence, which can worsen sleep apnea. Addressing nasal congestion is essential for individuals with sleep apnea, as it can improve the effectiveness of treatments and reduce the severity of apneas. If nasal congestion is a persistent issue, it’s important to consult with a healthcare provider or an otolaryngologist to identify the underlying cause and develop an appropriate treatment plan. By treating nasal congestion, you can improve sleep quality and the effectiveness of sleep apnea treatments.
6. Sleep Deprivation
The connection between sleep deprivation and sleep apnea is cyclical. Sleep apnea leads to fragmented and disrupted sleep, resulting in daytime sleepiness and fatigue. This exhaustion can, in turn, exacerbate sleep apnea symptoms, creating a feedback loop of worsening sleep quality. Addressing sleep deprivation requires a multifaceted approach that focuses on improving sleep hygiene, developing healthy sleep habits, and managing sleep disorders like sleep apnea. Consistently implementing these strategies can help improve sleep quality and reduce the impact of sleep deprivation on sleep apnea symptoms.
7. High Blood Pressure
The link between sleep apnea and high blood pressure (hypertension) is well-established. During apneas, the body experiences intermittent drops in oxygen levels, triggering a “fight or flight” response that raises blood pressure. Over time, these repeated episodes of high blood pressure can lead to chronic hypertension. Untreated high blood pressure can further exacerbate sleep apnea symptoms. Elevated blood pressure can cause changes in the structure of the blood vessels and the airway, making it more prone to collapse during sleep.
Managing both sleep apnea and high blood pressure is essential for overall health and well-being.
8. Family History and Genetics
Family history and genetics can influence your susceptibility to sleep apnea. Research indicates that sleep apnea tends to run in families, suggesting a genetic component to the condition. If you have close relatives, such as parents or siblings, with sleep apnea, you may be at an increased risk. While you cannot change your genetic makeup, understanding your family history can be valuable in managing sleep apnea.
Sleep apnea is a treatable condition, but it requires awareness and proactive management. Understanding the factors that can worsen sleep apnea is the first step toward effective treatment and improved sleep quality. If you suspect you have sleep apnea or are already diagnosed, consult with a healthcare professional or sleep specialist to develop a comprehensive plan tailored to your specific needs. By addressing these factors and working closely with your healthcare team, you can significantly improve your quality of life and reduce the impact of sleep apnea on your physical, emotional, and mental health.
Who Can I Contact With Questions?
At the Jacksonville Sleep Center, we are dedicated to providing personalized and effective solutions for individuals dealing with sleep apnea. Our team of experienced sleep specialists understands the complexities of sleep disorders, including sleep apnea, and offers comprehensive diagnostic evaluations to pinpoint the underlying causes of your condition. Whether it’s a sleep study to confirm the diagnosis or a tailored treatment plan that may involve therapies like CPAP, oral appliances, or lifestyle modifications, we’re here to guide you every step of the way. Our goal is to help you achieve restful and uninterrupted sleep, improving your overall well-being and quality of life. Your journey to better sleep begins with us.